How Smoking Affects Retinal Blood Flow and Vision
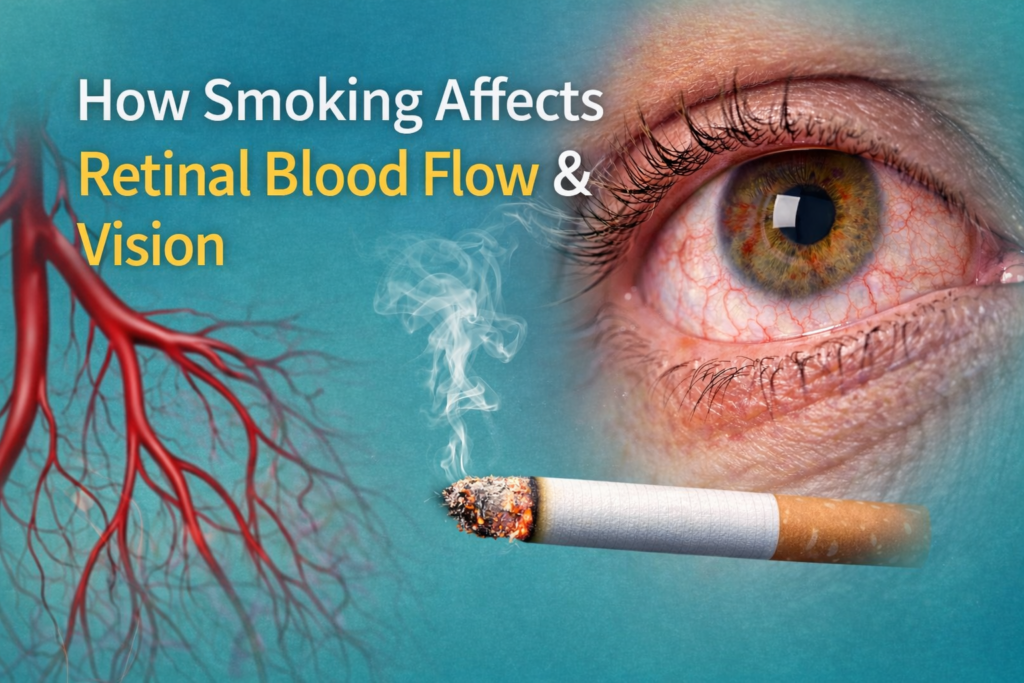
Smoking is widely known to harm the lungs and heart, but its damaging effects on eye health-especially the retina-are often overlooked. The retina is a highly sensitive tissue that depends on a rich and steady blood supply to function properly, and even minor disruptions can threaten vision. When smoking interferes with retinal blood flow, it can gradually impair vision and increase the risk of serious, sometimes irreversible eye diseases, making early evaluation by a Retina Specialist crucial. Understanding how smoking affects the retina is essential for protecting long-term vision and overall eye health. Understanding the Retina and Its Blood Supply The retina is a thin, light-sensitive layer of tissue lining the back of the eye. It plays a vital role in converting light into electrical signals that the brain interprets as vision. Because of its high metabolic activity, the retina requires a continuous supply of oxygen and nutrients delivered through a complex network of blood vessels. Even minor disruptions in retinal circulation can lead to cell damage. Over time, reduced blood flow may cause degeneration of retinal cells, resulting in blurred vision, blind spots, or permanent vision loss. This delicate balance makes the retina particularly vulnerable to the harmful effects of smoking. How Smoking Affects Blood Flow in the Retina Smoking introduces thousands of toxic chemicals into the bloodstream, many of which directly affect blood vessels. 1. Vasoconstriction and Reduced Oxygen Nicotine causes blood vessels to constrict, narrowing their diameter. When retinal blood vessels constrict, less oxygen-rich blood reaches the retinal tissue. This oxygen deprivation stresses retinal cells and reduces their ability to function normally. 2. Carbon Monoxide and Oxygen Deprivation Cigarette smoke contains carbon monoxide, which binds to hemoglobin more readily than oxygen. This reduces the amount of oxygen that red blood cells can deliver to tissues, including the retina. Chronic oxygen deprivation accelerates retinal damage and increases the risk of vascular complications. 3. Increased Blood Thickness Smoking can increase blood viscosity, making it thicker and more prone to clot formation. Thickened blood flows less efficiently through the tiny retinal capillaries, further reducing nutrient delivery and increasing the likelihood of blockages. Oxidative Stress and Retinal Damage Smoking is a major source of oxidative stress. Free radicals generated by tobacco smoke damage cells by altering their structure and function. The retina is especially susceptible to oxidative stress because of its high exposure to light and oxygen. Over time, oxidative damage can break down retinal cells, disrupt photoreceptors, and impair visual processing. This process plays a significant role in the development of several smoking-related retinal diseases. Smoking and Major Retinal Diseases 1. Age-Related Macular Degeneration (AMD) Smoking is one of the strongest modifiable risk factors for age-related macular degeneration. AMD affects the macula, the central part of the retina responsible for sharp, detailed vision. Smokers are significantly more likely to develop AMD and tend to experience faster disease progression than non-smokers. Damage to retinal blood vessels and increased oxidative stress caused by smoking accelerate macular degeneration, leading to difficulty reading, recognizing faces, and performing daily tasks. 2. Diabetic Retinopathy In people with diabetes, smoking worsens blood vessel damage throughout the body, including the retina. Smoking increases inflammation and impairs blood flow, intensifying the effects of high blood sugar on retinal vessels. This combination raises the risk of retinal bleeding, fluid leakage, and abnormal blood vessel growth. A Retina Specialist often emphasizes smoking cessation as a critical part of managing diabetic eye disease. 3. Retinal Vein and Artery Occlusion Smoking increases the risk of blood clots, which can block retinal veins or arteries. Retinal vein occlusion leads to swelling, bleeding, and sudden vision loss, while retinal artery occlusion is a medical emergency that can cause immediate and severe vision loss. Both conditions are closely linked to poor vascular health, making smokers particularly vulnerable. 4. Cataracts and Indirect Retinal Impact Although cataracts affect the lens rather than the retina, smoking-related cataracts reduce the amount of light reaching the retina. Over time, reduced visual input can affect retinal stimulation and overall visual quality, compounding vision problems. Long-Term Vision Effects of Smoking The effects of smoking on retinal blood flow are often gradual, which makes early damage easy to ignore. Many smokers do not notice symptoms until significant retinal injury has already occurred. Common long-term effects include: Once retinal cells are damaged or destroyed, they cannot regenerate. This is why early intervention and lifestyle changes are so important. Can Quitting Smoking Improve Retinal Health? The good news is that quitting smoking can significantly slow the progression of retinal damage. While some damage may be irreversible, smoking cessation improves blood circulation, reduces inflammation, and lowers oxidative stress throughout the body. Over time, improved oxygen delivery helps preserve remaining retinal cells and reduces the risk of further vision loss. Many patients who quit smoking experience better treatment outcomes when managing retinal diseases under the care of a Retina Specialist. Diagnosis and Monitoring of Smoking-Related Retinal Damage Detecting smoking-related retinal damage requires comprehensive eye examinations and advanced imaging techniques. Common diagnostic tools include: These tests help identify early vascular changes, swelling, or degeneration before severe vision loss occurs. Regular monitoring is especially important for smokers and former smokers. Treatment Options for Retinal Conditions in Smokers Treatment depends on the specific retinal condition and its severity. 1. Medications and Injections Anti-inflammatory and anti-VEGF injections may be used to reduce swelling and abnormal blood vessel growth in conditions such as diabetic retinopathy or macular degeneration. 2. Laser Therapy Laser treatment can help seal leaking blood vessels or prevent further retinal damage in certain vascular conditions. A Retina Specialist carefully determines whether laser therapy is appropriate based on individual retinal findings. 3. Surgical Intervention In advanced cases involving retinal detachment or severe bleeding, surgical procedures such as vitrectomy may be required to preserve vision. Regardless of treatment type, quitting smoking greatly improves the effectiveness of retinal therapies. Who Is at Highest Risk? Smoking-related retinal damage is more likely in individuals who: For these individuals, regular eye checkups are essential. Prevention:
Understanding the Retina: Functions, Problems & Eye Emergencies

The human eye is often compared to a camera, and at the heart of this comparison lies the retina. Though thin and delicate, the retina plays a critical role in vision, allowing us to see color, detail, light, and motion. Any damage or disease affecting the retina can have a serious impact on eyesight and, in some cases, lead to permanent vision loss, which is why timely evaluation by a Retina Specialist is so important. Understanding how the retina functions, the problems that can affect it, and the emergencies that require immediate care is essential for maintaining lifelong eye health. What Is the Retina? The retina is a thin layer of light-sensitive tissue located at the back of the eye. It receives light that enters through the cornea and lens, then converts that light into electrical signals. These signals are transmitted to the brain via the optic nerve, where they are interpreted as images. Types of Photoreceptor Cells in the Retina The retina contains two main types of photoreceptor cells: Because of its complex structure and essential function, even minor retinal damage can significantly affect visual clarity. Functions of the Retina The retina is far more than a passive screen at the back of the eye. It performs multiple critical functions that work together seamlessly. Light Detection and Signal Conversion The retina’s primary role is to detect light and convert it into neural signals. When light hits the photoreceptor cells, chemical changes occur that generate electrical impulses. These impulses travel through layers of retinal cells and ultimately reach the optic nerve. Color and Detail Perception Cone cells, which are concentrated in the central retina (macula), are responsible for sharp central vision and color discrimination. This is why the macula is essential for activities such as reading, driving, and recognizing faces. Peripheral and Night Vision Rod cells are more sensitive to light and are located mostly in the outer regions of the retina. They help us see in dim lighting and detect movement in our peripheral vision. Image Processing Before the Brain Interestingly, the retina performs a significant amount of image processing before the information ever reaches the brain. It adjusts for contrast, brightness, and movement, helping the brain receive a clearer and more usable visual signal. Common Retina Problems Retinal conditions can develop slowly or suddenly. Some are age-related, while others are linked to systemic diseases or trauma. Age-Related Macular Degeneration (AMD) AMD affects the macula and is one of the leading causes of vision loss in older adults. It can result in blurred or distorted central vision, making daily tasks difficult. Diabetic Retinopathy This condition occurs when high blood sugar levels damage the small blood vessels in the retina. Over time, these vessels may leak, swell, or close off completely, leading to vision impairment or blindness if untreated. Retinal Detachment A retinal detachment happens when the retina pulls away from its normal position. This is a medical emergency, as the retina cannot function properly when detached from its blood supply. Macular Edema Macular edema involves swelling in the macula due to fluid leakage. It is often associated with diabetes, retinal vein occlusion, or eye surgery. Retinal Vein Occlusion This condition occurs when a vein in the retina becomes blocked, leading to bleeding, swelling, and sudden vision loss. Many of these conditions require evaluation and management by a Retina Specialist with advanced diagnostic tools and treatment options. Retina Emergencies You Should Never Ignore Some retinal issues develop gradually, but others strike suddenly and require immediate medical attention. Knowing the warning signs can save your vision. Sudden Flashes and Floaters Seeing sudden flashes of light or a shower of floaters can be an early sign of retinal tears or detachment. While occasional floaters are common, a sudden increase should never be ignored. A Dark Curtain or Shadow If you notice a dark shadow or curtain moving across your field of vision, this may indicate retinal detachment. Immediate evaluation is critical to prevent permanent vision loss. Sudden Vision Loss Any sudden loss of vision, whether partial or complete, is considered an emergency. It may be caused by retinal artery occlusion, vein occlusion, or severe inflammation. Distorted or Wavy Vision When straight lines appear bent or wavy, it may signal macular involvement, such as macular edema or macular degeneration. In all these cases, prompt care from a Retina Specialist can make the difference between vision preservation and permanent damage. How Retina Conditions Are Diagnosed Modern eye care relies on advanced imaging and diagnostic techniques to evaluate retinal health accurately. Common Diagnostic Tools These tests help pinpoint the exact location and severity of retinal damage, allowing targeted treatment plans. Treatment Options for Retinal Diseases Treatment depends on the specific condition, its severity, and how early it is detected. Medications and Injections Many retinal conditions are treated with intravitreal injections that reduce inflammation, control abnormal blood vessel growth, or decrease fluid leakage. Laser Therapy Laser treatment may be used to seal leaking blood vessels, prevent abnormal vessel growth, or stabilize retinal tears before detachment occurs. Surgical Intervention Advanced surgeries such as vitrectomy or scleral buckle procedures may be required for retinal detachment or severe bleeding within the eye. These procedures are typically performed by a highly trained Retina Specialist. Ongoing Monitoring Some retinal diseases require long-term monitoring rather than immediate treatment. Regular follow-ups help track progression and adjust care as needed. Who Is at Higher Risk for Retina Problems? While anyone can develop retinal issues, certain factors increase risk: People in high-risk groups should have regular comprehensive eye exams to detect problems early. Preventing Retina Damage Although not all retinal conditions can be prevented, healthy habits can reduce risk and support overall eye health. Tips for Retinal Health Early detection remains one of the most powerful tools in preventing severe vision loss. When to See a Retina Specialist General eye exams are essential, but certain symptoms and conditions warrant specialized care. If you experience persistent vision changes, sudden visual disturbances, or have a known
Diabetes Eye Care Guide: Protect Vision | Retina Specialist

How Should Diabetes Patients Take Care of Their Eyes Diabetes is a chronic condition that affects millions of people worldwide. While most patients are aware of how diabetes impacts blood sugar levels, fewer realize how seriously it can affect eye health. Over time, uncontrolled diabetes can damage the delicate blood vessels in the eyes, leading to vision problems and, in severe cases, permanent blindness. The good news is that with proper care, regular check-ups, and guidance from a qualified Retina Specialist, most diabetes-related eye complications can be prevented or managed effectively. This blog explains how diabetes affects the eyes, common eye problems seen in diabetic patients, and practical steps to protect vision for the long term. Understanding the Link Between Diabetes and Eye Health Diabetes affects the body by increasing blood sugar levels, which can damage small blood vessels and nerves. The eyes are particularly vulnerable because the retina—the light-sensitive tissue at the back of the eye-depends on a healthy blood supply to function properly. When blood sugar remains high for long periods, it weakens retinal blood vessels, causing leakage, swelling, or abnormal new vessel growth. According to eye care professionals and every experienced Retina Specialist, diabetes is one of the leading causes of preventable blindness in adults. However, early detection and good diabetes control significantly reduce the risk. Common Eye Problems in Diabetes Patients 1. Diabetic Retinopathy Diabetic retinopathy is the most common diabetes-related eye disease. It occurs when high blood sugar damages the retinal blood vessels. In early stages, patients may not notice any symptoms, which is why regular eye exams are critical. As the condition progresses, symptoms may include: A Retina Specialist plays a key role in diagnosing and treating diabetic retinopathy before it causes irreversible damage. 2. Diabetic Macular Edema (DME) The macula is the central part of the retina responsible for sharp vision. When fluid leaks into this area, it causes swelling known as diabetic macular edema. This condition can severely affect reading, driving, and facial recognition. Early treatment under the care of a Retina Specialist can help preserve central vision. 3. Cataracts People with diabetes are more likely to develop cataracts at a younger age. Cataracts cause clouding of the eye’s natural lens, leading to blurry or dull vision. 4. Glaucoma Diabetes doubles the risk of glaucoma, a condition that damages the optic nerve due to increased eye pressure. Vision loss from glaucoma is permanent if not detected early. Importance of Regular Eye Examinations One of the most important steps diabetes patients can take is scheduling regular eye exams. Many diabetic eye diseases develop silently, without pain or early warning signs. Eye exam recommendations: Most eye doctors and Retina Specialist professionals recommend at least one comprehensive dilated eye exam every year. How Blood Sugar Control Protects Your Eyes Maintaining stable blood sugar levels is the foundation of diabetic eye care. Sudden spikes or long-term high glucose levels increase the risk of retinal damage. Tips for blood sugar control: Clinical studies consistently show that patients with well-controlled diabetes have a much lower risk of developing severe eye complications. Role of Diet in Diabetic Eye Health A healthy diet supports both blood sugar control and eye health. Nutrients that benefit the eyes include antioxidants, vitamins, and healthy fats. Eye-friendly foods for diabetes patients: Many Retina Specialist doctors emphasize that a nutrient-rich diet helps protect retinal cells from oxidative stress. Managing Blood Pressure and Cholesterol High blood pressure and cholesterol worsen diabetic eye disease by further damaging blood vessels. Keeping these under control helps maintain healthy circulation to the retina. Healthy habits include: Protecting Eyes from External Factors Diabetes can make eyes more sensitive to environmental stress. Simple protective steps: These habits support overall eye comfort and long-term vision health. Importance of Early Treatment and Monitoring If diabetic eye disease is detected early, treatments are highly effective. Modern ophthalmology offers advanced options such as: A qualified Retina Specialist determines the most suitable treatment based on disease stage and individual patient needs. Warning Signs Diabetes Patients Should Never Ignore Seek immediate medical attention if you notice: Prompt evaluation by a Retina Specialist can prevent permanent vision loss. Emotional and Lifestyle Impact of Vision Changes Vision problems can affect independence, work, and quality of life. Diabetes patients should not ignore emotional stress related to vision changes. Support from family, counseling, and medical professionals plays an important role in long-term care. When to See a Retina Specialist While general eye check-ups are essential, diabetes patients may need specialized retinal care. A Retina Specialist has advanced training in diagnosing and treating retinal diseases related to diabetes. Early referral ensures timely intervention and better outcomes. Final Thoughts Diabetes does not have to lead to vision loss. With proper blood sugar control, a healthy lifestyle, regular eye exams, and timely care from an experienced Retina Specialist, most diabetes-related eye complications can be prevented or effectively managed. Your eyes are precious. Taking proactive steps today-through awareness, nutrition, medical care, and routine monitoring-can help protect your vision for years to come. If you have diabetes, make eye care a priority, because early action is the key to lifelong healthy sight.
Summer Eye Health Foods for Strong Vision | Retina Specialist

Summer Season Eye Health: What to Eat for Stronger, Healthier Eyes Summer is a season of sunshine, outdoor activities, vacations, and longer days. While we often focus on protecting our skin during this time, eye health is frequently overlooked. Increased exposure to sunlight, heat, dust, dehydration, and screen time can strain your eyes and affect long-term vision if not managed properly. According to every experienced Retina Specialist, maintaining good eye health during summer isn’t just about wearing sunglasses-it also depends heavily on what you eat. How Summer Affects Eye Health Summer brings environmental challenges that can impact your eyes in several ways: 1. Increased UV Exposure Strong ultraviolet (UV) rays can damage sensitive eye tissues, including the retina. Prolonged exposure increases the risk of cataracts, macular degeneration, and retinal damage. 2. Dry Eyes and Dehydration Hot weather and excessive sweating can lead to dehydration, reducing tear production and causing dry, irritated eyes. 3. Dust, Pollution, and Allergens Summer winds often carry dust and allergens that can irritate the eyes, causing redness, itching, and infections. 4. More Screen Time Long summer evenings often mean increased screen usage-phones, tablets, and laptops-which can lead to digital eye strain. To counter these effects, eye protection and proper nutrition are equally important. Why Nutrition Is Essential for Eye Health Your eyes are complex organs that rely on vitamins, minerals, and antioxidants to stay healthy. A nutrient-rich diet helps: Many studies and clinical observations by Retina Specialist doctors confirm that people with balanced diets rich in eye-friendly nutrients have a lower risk of vision deterioration. Key Nutrients for Stronger, Healthier Eyes Before diving into specific foods, let’s understand the nutrients your eyes need most: 1. Vitamin A Essential for night vision and maintaining the cornea. 2. Vitamin C A powerful antioxidant that protects against UV damage. 3. Vitamin E Helps prevent oxidative damage to eye cells. 4. Lutein and Zeaxanthin Carotenoids that protect the retina from harmful blue light. 5. Omega-3 Fatty Acids Reduce dry eyes and support retinal function. 6. Zinc Helps transport Vitamin A to the retina for melanin production. Best Summer Foods for Eye Health 1. Carrots Carrots are rich in beta-carotene, which the body converts into Vitamin A. This vitamin is essential for maintaining good vision, especially in low-light conditions. How to eat in summer: Eye doctors and Retina Specialist experts often recommend carrots as a foundational food for eye health. 2. Leafy Green Vegetables Spinach, kale, and lettuce are packed with lutein and zeaxanthin, which protect the retina from UV damage and oxidative stress. Benefits: Summer tip: Add fresh greens to smoothies or light salads. 3. Citrus Fruits Oranges, lemons, grapefruits, and sweet limes are rich in Vitamin C, which strengthens blood vessels in the eyes and reduces the risk of cataracts. Easy summer options: A balanced intake of citrus fruits is frequently suggested by every experienced Retina Specialist for maintaining long-term eye health. 4. Berries Strawberries, blueberries, blackberries, and raspberries contain antioxidants that fight free radicals and protect retinal cells. Why berries are great: Enjoy them chilled for a refreshing summer snack. 5. Fatty Fish Salmon, tuna, sardines, and mackerel are rich in omega-3 fatty acids, which are crucial for retinal health and tear production. Benefits: According to leading Retina Specialist doctors, omega-3 deficiency is a common cause of dry eye syndrome. 6. Eggs Egg yolks are an excellent source of lutein, zeaxanthin, zinc, and Vitamin A. Why eggs matter: Eggs are easy to digest and suitable for all age groups during summer. 7. Nuts and Seeds Almonds, walnuts, sunflower seeds, and flaxseeds provide Vitamin E and omega-3 fatty acids. Benefits: A small handful daily can make a big difference. 8. Watermelon Watermelon is rich in water content and contains Vitamin A and C. Summer advantage: Hydration is often emphasized by Retina Specialist professionals as a simple yet powerful step for eye comfort. 9. Bell Peppers Red, yellow, and green bell peppers are packed with Vitamin C and beta-carotene. Why include them: They’re perfect for summer stir-fries and salads. 10. Cucumbers Cucumbers are hydrating and soothing, making them excellent for eye health. Benefits: Add them to salads or infused water. Summer Eye Care Tips Along with Diet Nutrition works best when combined with healthy habits: Most Retina Specialist doctors agree that lifestyle choices can significantly impact how well your eyes age. When to Consult an Eye Specialist If you experience symptoms like persistent dryness, blurred vision, eye pain, floaters, or light sensitivity, don’t ignore them. Early diagnosis and timely care from a qualified Retina Specialist can prevent serious eye conditions and preserve vision. Final Thoughts Summer is the perfect time to nourish your body-and your eyes-with fresh, colorful, nutrient-rich foods. A diet rich in fruits, vegetables, healthy fats, and hydration can go a long way in protecting your vision from seasonal stress and long-term damage. By making smart dietary choices and following simple eye care habits, you can enjoy clearer, stronger, and healthier vision all summer long. And remember, regular eye check-ups and guidance from a trusted Retina Specialist are essential for maintaining lifelong eye health.
Contact Lens Users: 7 Eye Care Mistakes | Laser Eye Treatment
Contact Lens Users: 7 Eye Care Mistakes You Should Avoid Contact lenses offer freedom from glasses and provide clear, comfortable vision for millions of people worldwide. However, improper contact lens habits can lead to serious eye problems, including infections, irritation, and long-term vision damage. Many contact lens users unknowingly make small mistakes in their daily routines that can negatively affect their eye health over time. In some cases, repeated issues may even push people to explore alternatives such as laser eye treatment, making prevention and proper care even more important. If you wear contact lenses or are considering them, understanding these common eye care mistakes can help protect your vision and keep your eyes healthy for years to come. Why Proper Contact Lens Care Matters Your eyes are extremely sensitive organs. Contact lenses sit directly on the eye’s surface, which means even minor hygiene lapses can allow bacteria, fungi, or debris to enter the eye. Poor lens care can result in dryness, redness, blurred vision, and painful infections like keratitis. Many people only realize the seriousness of these issues when discomfort becomes constant or vision begins to suffer. While advanced solutions such as laser eye treatment exist for vision correction, prevention remains the best approach. Maintaining good contact lens hygiene reduces the risk of complications and preserves overall eye health. Mistake 1: Sleeping with Contact Lenses On One of the most common and dangerous mistakes contact lens users make is sleeping while wearing their lenses. Even if the lenses feel comfortable, sleeping in them significantly increases the risk of eye infections. When your eyes are closed, oxygen supply to the cornea decreases. Contact lenses further reduce oxygen flow, creating a breeding ground for bacteria. This can lead to redness, pain, light sensitivity, and even corneal ulcers. What to do instead: Always remove your contact lenses before sleeping unless your eye doctor has specifically prescribed extended-wear lenses and given clear instructions for their use. Mistake 2: Poor Hand Hygiene Before Handling Lenses Touching contact lenses with unwashed hands introduces germs directly into your eyes. Many users rinse their hands quickly or skip washing altogether, especially when they are in a hurry. This habit can transfer dirt, oils, and harmful microorganisms to the lens surface, increasing the risk of infection and irritation. What to do instead: Wash your hands thoroughly with soap and water before handling contact lenses. Dry them with a lint-free towel to prevent fibers from sticking to the lenses. Mistake 3: Overusing Contact Lenses Beyond Their Schedule Contact lenses are designed for specific usage periods—daily, bi-weekly, or monthly. Wearing lenses longer than recommended can cause protein deposits and bacteria to build up, even if the lenses appear clean. Overuse reduces oxygen flow to the eyes and can worsen dryness, redness, and blurred vision. Chronic misuse may damage the cornea and affect long-term eye health, sometimes prompting people to consider permanent solutions like laser eye treatment earlier than expected. What to do instead: Follow the replacement schedule exactly as prescribed. Set reminders if necessary, and never stretch lens usage to save money. Mistake 4: Using Water or Saliva to Clean Lenses Some contact lens users rinse lenses with tap water or saliva when lens solution is unavailable. This is extremely dangerous. Tap water can contain microorganisms, including Acanthamoeba, which can cause severe and painful eye infections. Saliva is also full of bacteria and enzymes that can damage lenses and irritate the eyes. What to do instead: Always use sterile contact lens solution recommended by your eye care professional. Never expose lenses to water, including swimming pools, showers, or hot tubs. Mistake 5: Ignoring Eye Discomfort and Redness Many people continue wearing contact lenses despite experiencing burning, itching, or redness, assuming the symptoms will resolve on their own. Ignoring these warning signs can worsen underlying problems and lead to serious complications. Persistent discomfort may indicate dryness, infection, or improper lens fit. Long-term irritation can cause scarring or vision changes that may require medical intervention. What to do instead: If discomfort persists, stop wearing your lenses immediately and consult an eye doctor. Early treatment can prevent complications and help preserve your vision. Mistake 6: Skipping Regular Eye Check-Ups Once people get comfortable with contact lenses, they often skip routine eye exams. However, regular check-ups are essential for monitoring eye health and ensuring that your lenses still fit properly. Changes in vision, tear production, or eye shape can occur over time, making previously comfortable lenses unsuitable. Regular exams also help detect early signs of infection or dryness before symptoms worsen. Some individuals who experience recurring contact lens issues begin exploring alternatives such as laser eye treatment, but even then, proper evaluation and guidance from an eye specialist are crucial. What to do instead: Schedule regular eye exams as recommended by your eye care professional, even if your vision feels fine. Mistake 7: Wearing Contact Lenses for Too Many Hours a Day Wearing contact lenses for extended periods without breaks can strain the eyes and worsen dryness. Long screen time combined with contact lens wear further reduces blinking, leading to increased discomfort and fatigue. Chronic dryness and irritation may eventually make contact lens wear intolerable for some users, pushing them toward options like laser eye treatment for long-term relief. What to do instead: Give your eyes regular breaks. Switch to glasses for part of the day, especially during long screen sessions or when your eyes feel tired. Long-Term Impact of Poor Contact Lens Habits Repeated contact lens mistakes don’t just cause temporary discomfort- they can have lasting effects on eye health. Chronic dryness, corneal damage, and recurring infections can affect vision quality and overall eye comfort. For some people, these issues lead to reduced tolerance for contact lenses altogether. In such cases, vision correction alternatives like laser eye treatment may be considered, but eligibility depends on eye health, corneal thickness, and medical history. Maintaining healthy contact lens habits can help delay or even eliminate the need for such interventions. Tips for Healthy Contact
Dry Eye Syndrome Explained: Causes, Symptoms, and Modern Treatments
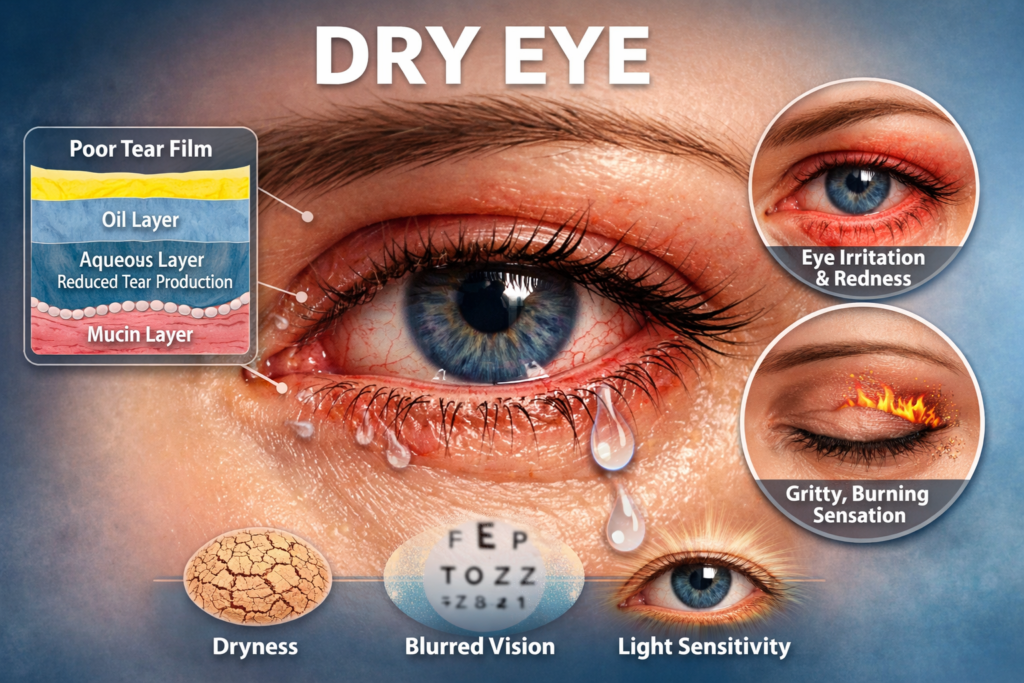
Dry Eye Syndrome: Causes, Symptoms, and Treatment Dry Eye Syndrome is one of the most common yet often underestimated eye conditions affecting millions of people worldwide. Characterized by insufficient tear production or poor tear quality, this condition can significantly impact daily comfort, vision clarity, and overall quality of life. While it may sound minor, untreated dry eye can lead to chronic irritation, inflammation, and even damage to the eye’s surface. Understanding its causes, recognizing early symptoms, and knowing the available treatment options are essential steps toward long-term eye health. In some cases, consulting an eye care professional such as a retina specialist may be crucial for accurate diagnosis and comprehensive management. What Is Dry Eye Syndrome? Dry Eye Syndrome, also known as keratoconjunctivitis sicca, occurs when the eyes do not produce enough tears or when tears evaporate too quickly. Tears are not just water; they are a complex mixture of water, oils, and mucus that work together to keep the surface of the eye smooth, nourished, and protected. When this balance is disrupted, the eyes become dry, irritated, and vulnerable to inflammation and infection. The condition can be temporary or chronic. Environmental factors may cause short-term dryness, while underlying health issues can result in long-lasting symptoms. Because dry eye symptoms often worsen gradually, many people dismiss them until they begin interfering with reading, driving, or screen use. Causes of Dry Eye Syndrome Dry Eye Syndrome can develop due to a wide range of factors, often overlapping with one another. Understanding the root cause is essential for effective treatment. 1. Reduced Tear Production As people age, tear production naturally decreases. This is especially common after the age of 50. Certain medical conditions such as diabetes, thyroid disorders, rheumatoid arthritis, and lupus can also reduce tear output. In such cases, an ophthalmologist or retina specialist may work alongside other healthcare providers to manage both systemic disease and eye symptoms. 2. Increased Tear Evaporation Even if tear production is normal, tears may evaporate too quickly. This can occur due to: Modern lifestyles, especially heavy digital device usage, have made evaporative dry eye increasingly common across all age groups. 3. Poor Tear Quality Healthy tears consist of three layers: lipid (oil), aqueous (water), and mucin. If any of these layers are deficient, tears become unstable. Meibomian gland dysfunction, a condition where oil glands in the eyelids do not function properly, is a major contributor to poor tear quality. 4. Medications Many commonly prescribed medications can contribute to dry eyes, including antihistamines, antidepressants, blood pressure medications, and hormonal treatments. Long-term use can exacerbate symptoms if not properly managed. Common Symptoms of Dry Eye Syndrome Dry Eye Syndrome presents with a variety of symptoms that can range from mild discomfort to persistent pain. These symptoms may affect one or both eyes and often worsen as the day progresses. When symptoms persist or affect vision quality, it is important to seek professional evaluation. In some cases, a retina specialist may be involved to rule out retinal or ocular surface complications, particularly in patients with diabetes or other systemic conditions. How Dry Eye Syndrome Is Diagnosed Diagnosing Dry Eye Syndrome involves a combination of symptom assessment and clinical tests. Eye care professionals may perform: Advanced diagnostic tools can also analyze tear composition and inflammation levels. A comprehensive eye exam ensures that symptoms are not caused by more serious underlying conditions, which is why collaboration with a retina specialist may be recommended for complex cases. Treatment Options for Dry Eye Syndrome Treatment for Dry Eye Syndrome is highly individualized and depends on the severity and underlying cause of the condition. The goal is to restore tear balance, reduce inflammation, and protect the ocular surface. 1. Artificial Tears and Lubricants Over-the-counter artificial tears are often the first line of treatment. Preservative-free options are preferred for frequent use. These drops help supplement natural tears and provide temporary relief. 2. Prescription Medications For moderate to severe dry eye, prescription eye drops may be used to reduce inflammation and increase tear production. These medications are typically used long-term under medical supervision. 3. Lifestyle and Environmental Adjustments Simple changes can make a significant difference: 4. Eyelid and Gland Treatments Warm compresses, lid hygiene routines, and in-office procedures can help improve oil gland function. These treatments are particularly effective for evaporative dry eye. 5. Advanced and Specialized Care In severe or complicated cases, treatment may require advanced therapies or multidisciplinary care. A retina specialist may be consulted if dry eye coexists with retinal diseases, post-surgical complications, or systemic health issues affecting eye function. Prevention and Long-Term Management While Dry Eye Syndrome cannot always be prevented, proactive care can significantly reduce its impact. Long-term management focuses on consistency and early intervention. Patients with diabetes, autoimmune disorders, or a history of eye surgery should be particularly vigilant, as they may require ongoing monitoring by both a general ophthalmologist and a retina specialist. When to See a Doctor You should seek professional care if dry eye symptoms: Ignoring symptoms can lead to corneal damage and increased risk of infection. Early diagnosis allows for more effective treatment and helps prevent long-term complications. Conclusion Dry Eye Syndrome is a common but complex condition that affects people of all ages. While symptoms may start as mild irritation, they can progress into chronic discomfort and vision problems if left untreated. Understanding the causes, recognizing early warning signs, and following a personalized treatment plan are key to maintaining healthy eyes. With proper care, lifestyle adjustments, and guidance from qualified eye care professionals—including, when necessary, a retina specialist – most people can successfully manage dry eye and protect their long-term vision.
