Dry Eye Syndrome: Causes, Symptoms, and Treatment
Dry Eye Syndrome is one of the most common yet often underestimated eye conditions affecting millions of people worldwide. Characterized by insufficient tear production or poor tear quality, this condition can significantly impact daily comfort, vision clarity, and overall quality of life. While it may sound minor, untreated dry eye can lead to chronic irritation, inflammation, and even damage to the eye’s surface. Understanding its causes, recognizing early symptoms, and knowing the available treatment options are essential steps toward long-term eye health. In some cases, consulting an eye care professional such as a retina specialist may be crucial for accurate diagnosis and comprehensive management.
What Is Dry Eye Syndrome?
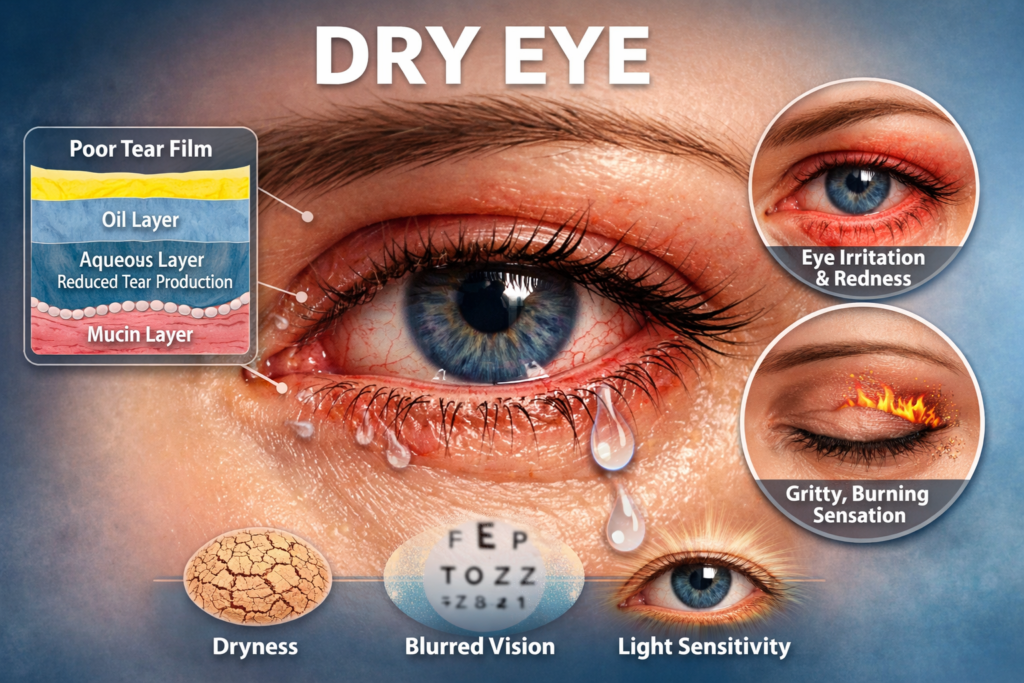
Dry Eye Syndrome, also known as keratoconjunctivitis sicca, occurs when the eyes do not produce enough tears or when tears evaporate too quickly. Tears are not just water; they are a complex mixture of water, oils, and mucus that work together to keep the surface of the eye smooth, nourished, and protected. When this balance is disrupted, the eyes become dry, irritated, and vulnerable to inflammation and infection.
The condition can be temporary or chronic. Environmental factors may cause short-term dryness, while underlying health issues can result in long-lasting symptoms. Because dry eye symptoms often worsen gradually, many people dismiss them until they begin interfering with reading, driving, or screen use.
Causes of Dry Eye Syndrome
Dry Eye Syndrome can develop due to a wide range of factors, often overlapping with one another. Understanding the root cause is essential for effective treatment.
1. Reduced Tear Production
As people age, tear production naturally decreases. This is especially common after the age of 50. Certain medical conditions such as diabetes, thyroid disorders, rheumatoid arthritis, and lupus can also reduce tear output. In such cases, an ophthalmologist or retina specialist may work alongside other healthcare providers to manage both systemic disease and eye symptoms.
2. Increased Tear Evaporation
Even if tear production is normal, tears may evaporate too quickly. This can occur due to:
- Prolonged screen use causing reduced blinking
- Exposure to wind, smoke, or dry climates
- Eyelid problems that prevent proper blinking
Modern lifestyles, especially heavy digital device usage, have made evaporative dry eye increasingly common across all age groups.
3. Poor Tear Quality
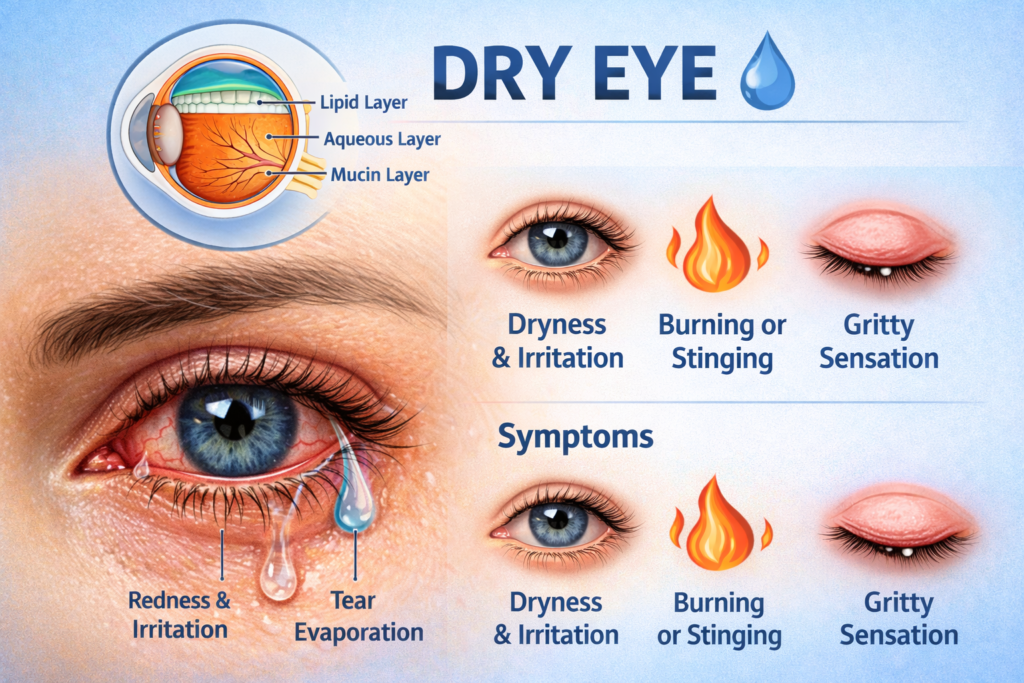
Healthy tears consist of three layers: lipid (oil), aqueous (water), and mucin. If any of these layers are deficient, tears become unstable. Meibomian gland dysfunction, a condition where oil glands in the eyelids do not function properly, is a major contributor to poor tear quality.
4. Medications
Many commonly prescribed medications can contribute to dry eyes, including antihistamines, antidepressants, blood pressure medications, and hormonal treatments. Long-term use can exacerbate symptoms if not properly managed.
Common Symptoms of Dry Eye Syndrome

Dry Eye Syndrome presents with a variety of symptoms that can range from mild discomfort to persistent pain. These symptoms may affect one or both eyes and often worsen as the day progresses.
- Burning, stinging, or scratchy sensation
- Redness and inflammation
- Sensitivity to light
- Blurred or fluctuating vision
- Feeling like something is stuck in the eye
- Excessive tearing (a reflex response to dryness)
When symptoms persist or affect vision quality, it is important to seek professional evaluation. In some cases, a retina specialist may be involved to rule out retinal or ocular surface complications, particularly in patients with diabetes or other systemic conditions.
How Dry Eye Syndrome Is Diagnosed
Diagnosing Dry Eye Syndrome involves a combination of symptom assessment and clinical tests. Eye care professionals may perform:
- Tear break-up time tests to measure tear stability
- Schirmer’s test to evaluate tear production
- Ocular surface staining to detect damage
- Meibomian gland evaluation
Advanced diagnostic tools can also analyze tear composition and inflammation levels. A comprehensive eye exam ensures that symptoms are not caused by more serious underlying conditions, which is why collaboration with a retina specialist may be recommended for complex cases.
Treatment Options for Dry Eye Syndrome
Treatment for Dry Eye Syndrome is highly individualized and depends on the severity and underlying cause of the condition. The goal is to restore tear balance, reduce inflammation, and protect the ocular surface.
1. Artificial Tears and Lubricants
Over-the-counter artificial tears are often the first line of treatment. Preservative-free options are preferred for frequent use. These drops help supplement natural tears and provide temporary relief.
2. Prescription Medications
For moderate to severe dry eye, prescription eye drops may be used to reduce inflammation and increase tear production. These medications are typically used long-term under medical supervision.
3. Lifestyle and Environmental Adjustments
Simple changes can make a significant difference:
- Taking regular breaks during screen use
- Using humidifiers in dry environments
- Wearing wraparound sunglasses outdoors
- Staying well hydrated
4. Eyelid and Gland Treatments
Warm compresses, lid hygiene routines, and in-office procedures can help improve oil gland function. These treatments are particularly effective for evaporative dry eye.
5. Advanced and Specialized Care
In severe or complicated cases, treatment may require advanced therapies or multidisciplinary care. A retina specialist may be consulted if dry eye coexists with retinal diseases, post-surgical complications, or systemic health issues affecting eye function.
Prevention and Long-Term Management
While Dry Eye Syndrome cannot always be prevented, proactive care can significantly reduce its impact. Long-term management focuses on consistency and early intervention.
- Schedule regular eye exams, especially if you have chronic health conditions
- Follow prescribed treatment plans even when symptoms improve
- Maintain good eyelid hygiene
- Limit exposure to known environmental triggers
Patients with diabetes, autoimmune disorders, or a history of eye surgery should be particularly vigilant, as they may require ongoing monitoring by both a general ophthalmologist and a retina specialist.
When to See a Doctor
You should seek professional care if dry eye symptoms:
- Persist for more than a few weeks
- Interfere with daily activities
- Cause pain or significant vision changes
Ignoring symptoms can lead to corneal damage and increased risk of infection. Early diagnosis allows for more effective treatment and helps prevent long-term complications.
Conclusion
Dry Eye Syndrome is a common but complex condition that affects people of all ages. While symptoms may start as mild irritation, they can progress into chronic discomfort and vision problems if left untreated. Understanding the causes, recognizing early warning signs, and following a personalized treatment plan are key to maintaining healthy eyes. With proper care, lifestyle adjustments, and guidance from qualified eye care professionals—including, when necessary, a retina specialist – most people can successfully manage dry eye and protect their long-term vision.